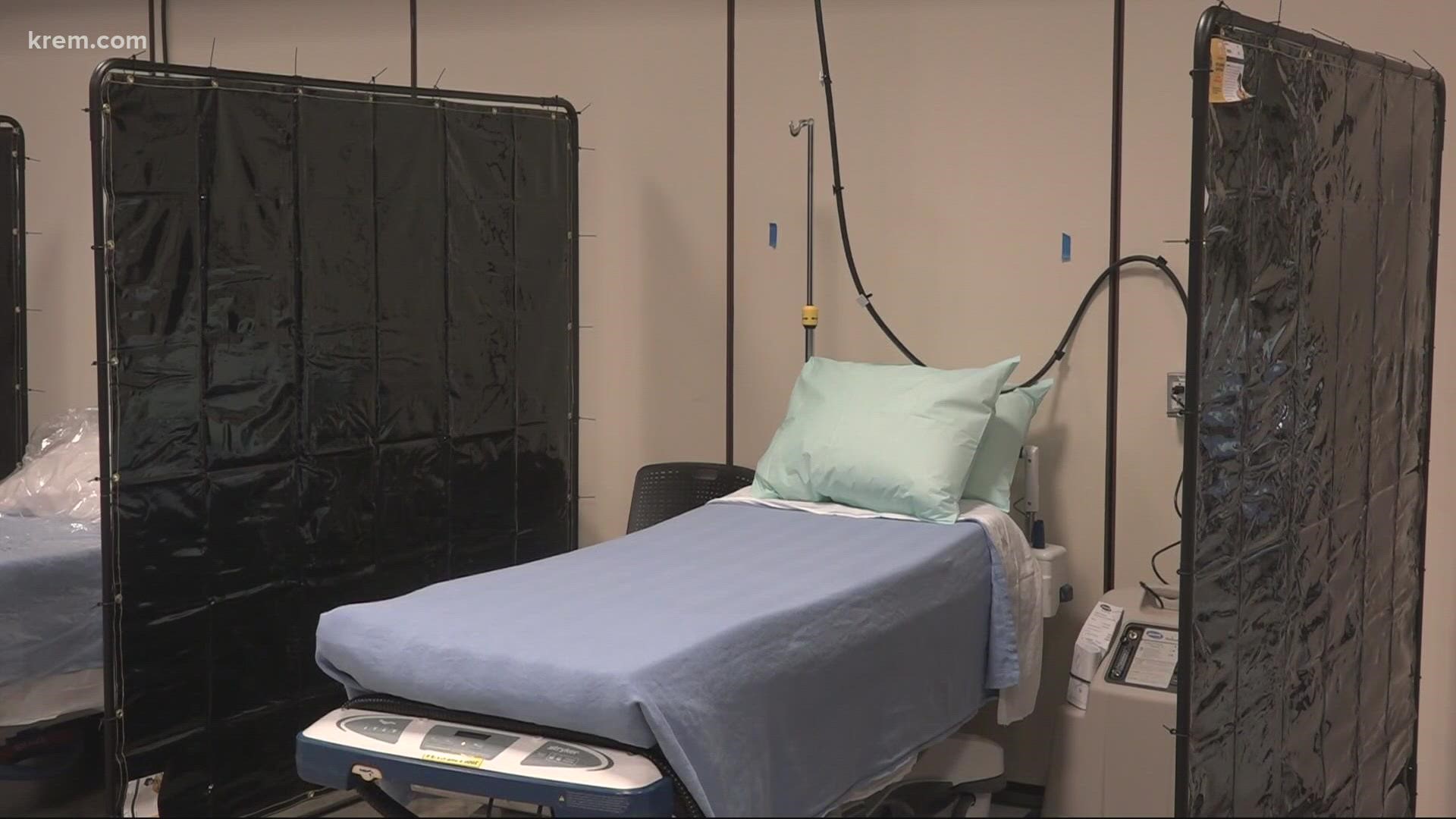
COEUR D'ALENE, Idaho — Kootenai Health started seeing patients in its Health Resource Center on Monday as the state transitions into Crisis Standards of Care in north and central Idaho.
Kootenai Health leaders made the decision on Aug. 20 to convert the hospital's largest conference room in the Health Resource Center into a patient care area dedicated to COVID-19 patients. Seven patients were moved into the Health Resource Center COVID-19 unit late Monday afternoon. It can accommodate up to 22 patients, according to the hospital.
Kootenai Health officials said in addition to elective surgeries, some more necessary procedures are now being postponed. This comes as doctors say resources are being stretched to their limits.
Kootenai Health Chief of Staff Dr. Robert Scoggins said during a press conference on Tuesday that the hospital caring for the largest number of COVID-19 patients its handled since the pandemic began, with 113 total and 39 in critical care. Nineteen patients are on ventilators.
"The message that I'd like to send to people is that, we're, you know, we're at the limit of what we can handle at this facility. We've done a lot of things to expand our care to take care of more patients, but we just, it keeps growing," Scoggins said.
Separate rooms in the Health Resource Center are being used to provide monoclonal antibody therapy to COVID-19 patients who are not hospitalized.
In a press release Tuesday, Kootenai Health said it has stretched existing staff, hired additional contract nurses, expanded bed capacity, canceled elective surgeries and adjusted contingency levels of care to accommodate the COVID-19 patient surges and volume demands. The hospital is scheduled to receive additional staffing from the Department of Defense and ACI Federal, which provides health care staffing on behalf of the federal government.
The Idaho Department of Health and Welfare activated crisis standards of care for hospitals in North Idaho Tuesday morning after a surge in COVID-19 cases left too few hospital beds and medical personnel to care for all the sick.
Kootenai Health said hospital leaders participated on the Idaho Crisis Standards of Care taskforce, and the hospital submitted a request to the state on Monday to activate Crisis Standards of Care.
North Idaho is the first region to put crisis standards in place, although doctors in the Treasure Valley have warned repeatedly that those extreme measures could be put in place statewide if Idahoans do not act to stem the tide of infections
Patients near death may only receive 'comfort care'
In the hard-hit region, which has Idaho's lowest rates of vaccination against COVID-19, someone struggling to breathe may no longer get a ventilator. Someone badly hurt in a car wreck or accident may no longer get a bed in the hospital. Someone near death from illness may receive only "comfort care" as hospital staff use limited medicine and life-saving equipment on patients likelier to pull through.
“We have reached an unprecedented and unwanted point in the history of our state. We have taken so many steps to avoid getting here, but yet again we need to ask more Idahoans to choose to receive the COVID-19 vaccine," Idaho Gov. Brad Little said. "More Idahoans need to choose to receive the vaccine so we can minimize the spread of the disease and reduce the number of COVID-19 hospitalizations, many of which involve younger Idahoans and are preventable with safe and effective vaccines."
More than 95% of COVID-19 patients in Idaho hospitals are unvaccinated.
IDHW officials say the vote to activate crisis standards of care came amid a "severe shortage of staffing and available beds" and a "massive increase in patients with COVID-19 who require hospitalization."
Under crisis standards, hospital beds, medicine, and equipment like ventilators may be allocated to those deemed most likely to survive, with the goal of saving as many lives as possible under extraordinary circumstances.
“Crisis standards of care is a last resort. It means we have exhausted our resources to the point that our healthcare systems are unable to provide the treatment and care we expect,” said DHW Director Dave Jeppesen. “This is a decision I was fervently hoping to avoid. The best tools we have to turn this around is for more people to get vaccinated and to wear masks indoors and in outdoor crowded public places. Please choose to get vaccinated as soon as possible – it is your very best protection against being hospitalized from COVID-19.”