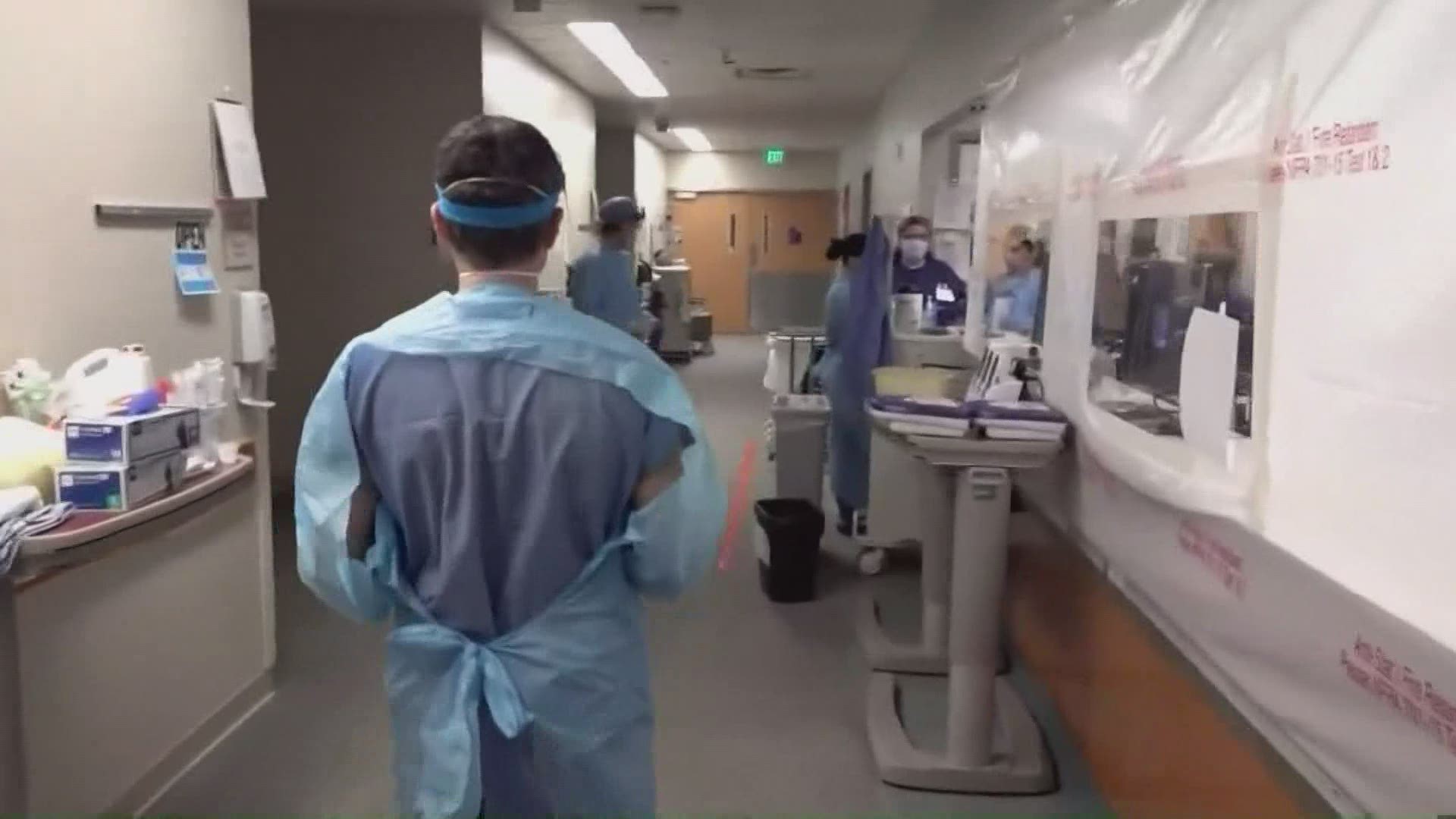
SEATTLE — The Washington health care system continues to be strapped for beds, staffing and all-around occupancy as the COVID-19 pandemic heads toward its third year.
But hospital leaders aren’t blaming COVID-19 patients for current occupancy issues, which have several major hospitals at or near 120% occupancy.
They’re blaming the fact that they can’t discharge many patients who shouldn’t even be in the hospital.
Executive Vice President of the Washington State Hospital Association (WSHA) Taya Briley explained the situation during a Monday briefing.
“Our hospitals are bursting at the seams,” she said. “But they're not filled with COVID-19 patients. Remarkably, they are filled with patients who do not need hospital care.”
Briley described the patients that hospitals can’t be moved out of hospitals as those who have “complex, long-term care needs,” for which a facility can’t be found due to staffing shortages.
Additionally, Briley said the process for patients to get evaluated and placed in facilities outside of a hospital by the state’s Medicaid program can take weeks and months.
Also, some of these patients qualify for a post-hospital treatment facility for things like dementia or other mental health needs but they don’t have a family member authorized to consent to their transfer.
“State law for family consent to long-term care placement is remarkably complex,” Briley said.
The fear for Briley and other hospital leaders is that a COVID-19 surge from the new omicron variant could create a situation where facilities must ration care.
“This is ironic because the patients who are in the hospital taking up the beds don't need acute care at all,” Briley said.
Chief Medical Officer of Providence Everett Jay Cook explained how the occupancy issue is already affecting his facility, which had to postpone 40 non-emergent but medically necessary surgeries just last week.
“Our team works really hard to get these cases scheduled as soon as possible, but in the meantime, patients and their families face the emotional and physical stress of having to wait for their procedure or service,” Cook said. “For example, last week, patients had to wait for a delayed heart valve replacement and for removal of cancerous tumors involving the colon.”
Briley said that to help the situation, WSHA is working with the state and long-term health care providers to implement solutions.
WSHA is looking for three things to develop and come out of the next state legislative session, as well, which takes place in January 2022.
First, WSHA is asking for legislation to smooth the consent process for patients that can be moved to long-term care. “Right now, a complex, expensive and court-intensive guardianship process is required,” she said.
WSHA is also asking the state to deploy resources to complete evaluations and streamline processes for patients awaiting transfers to other in-patient facilities.
Third, WSHA is asking the state to give more funding for those working in long-term care facilities.
While the week after Thanksgiving saw a small uptick in COVID-19 cases and hospitalizations, trends are mostly flat with about an average of 65 new COVID-19 hospitalizations and 12-20 deaths ever day across the state.
To prepare for a potential surge from the omicron variant, health leaders are urging everyone to get vaccinated and their booster shots, if eligible.